Chapter 10.pdf
CHAPTER 10 - TABLE OF CONTENTS 10.0 PURPOSE . 10-1 10.1 REFERENCE SUMMARY . 10-1 10.1.1 OPNAVINST 5100.23 (SERIES) . 10-1 10.1.2 GENERAL INDUSTRY OCCUPATIONAL SAFETY AND HEALTH STANDARDS (29 CFR Parts 1910.1 to end). 10-1 10.1.3 OPNAVINST 4110.2 (SERIES) . 10-1 10.1.4 NAVSECGRUINST 4110.2 (SERIES) . 10-2 10.1.5 OPNAVINST 5100.19 (SERIES) . 10-2 10.1.6 OPNAVINST 3120.32 (SERIES) . 10-2 10.2 SY
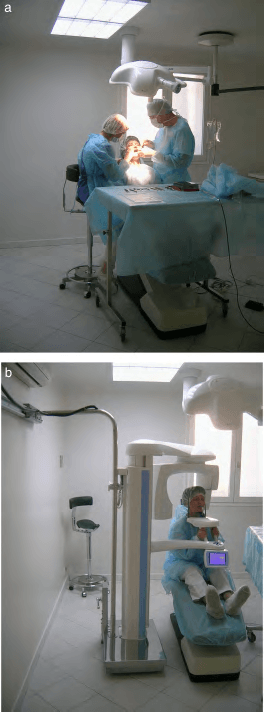
 Bousquet & Joyard . Surgical navigation for implant placement using transtomography
els), enhanced resolution (one picture pixelequals three physical pixels) and high re-solution (one picture pixel equals two phy-sical pixels). The size of the physical pixelis 33 mm. After picture calibration (1.4magnification coefficient in case of trans-tomography), measurements are then ta-ken with a 132 mm (33 Â 4) measurementunit in the normal resolution mode. Thisexplains why all the measurements (dis-tance and angle) of this study appear withinabout one-hundredth of a millimetre.
Bousquet & Joyard . Surgical navigation for implant placement using transtomography
els), enhanced resolution (one picture pixelequals three physical pixels) and high re-solution (one picture pixel equals two phy-sical pixels). The size of the physical pixelis 33 mm. After picture calibration (1.4magnification coefficient in case of trans-tomography), measurements are then ta-ken with a 132 mm (33 Â 4) measurementunit in the normal resolution mode. Thisexplains why all the measurements (dis-tance and angle) of this study appear withinabout one-hundredth of a millimetre.
 Bousquet & Joyard . Surgical navigation for implant placement using transtomography
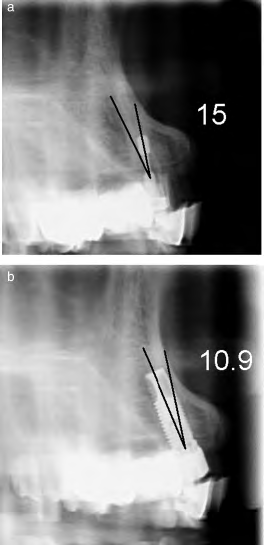
Fig. 5. (a) Case 5–intraoperative control–a 151 palatalrectification has to be carried out.(b) Case 5–post-operative control: effective rectification is 10.91.
Bousquet & Joyard . Surgical navigation for implant placement using transtomography
Fig. 5. (a) Case 5–intraoperative control–a 151 palatalrectification has to be carried out.(b) Case 5–post-operative control: effective rectification is 10.91.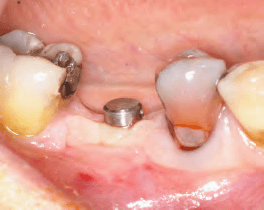 Bousquet & Joyard . Surgical navigation for implant placement using transtomography
Table 5. Deviation analysis – Statistics
Minimal value Maximal value Mean value Ecartype
that this procedure is as accurate as other
guidance systems, more flexible than tem-plate systems and has a favourable cost/
This technique appears to be suitable only
benefit ratio if we consider that the panora-
for small sectorial edentulism because of the
mic machine is also used for preplanning.
Bousquet & Joyard . Surgical navigation for implant placement using transtomography
Table 5. Deviation analysis – Statistics
Minimal value Maximal value Mean value Ecartype
that this procedure is as accurate as other
guidance systems, more flexible than tem-plate systems and has a favourable cost/
This technique appears to be suitable only
benefit ratio if we consider that the panora-
for small sectorial edentulism because of the
mic machine is also used for preplanning.