Unrelated donor and hla-identical sibling haematopoietic stem cell transplantation cure chronic granulomatous disease with good long-term outcome and growth
Unrelated donor and HLA-identical sibling haematopoieticstem cell transplantation cure chronic granulomatous diseasewith good long-term outcome and growthLaura B. K. R. Jones,1 Stephen Hughes,1Stephen Hodges,2 Terence J. Flood,1Chronic granulomatous disease (CGD) causes recurrent infection andexperience frequent hospitalisations and 50% mortality by 30 years. Haematopoietic stem cell trans
 Lactational mastitis
Lactational mastitis 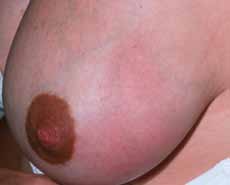
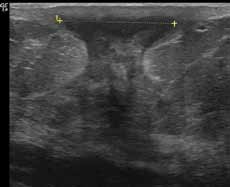 Lactational mastitis and breast abscess – diagnosis and management in general practice CLINICAL
Lactational mastitis and breast abscess – diagnosis and management in general practice CLINICAL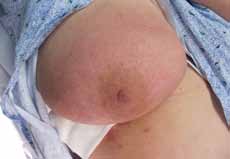 CLINICAL Lactational mastitis and breast abscess – diagnosis and management in general practice
CLINICAL Lactational mastitis and breast abscess – diagnosis and management in general practice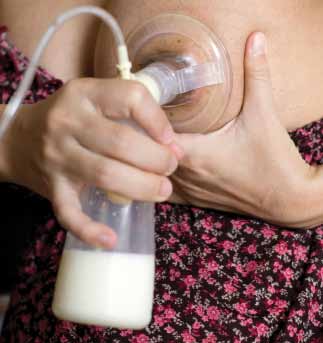 Lactational mastitis and breast abscess – diagnosis and management in general practice CLINICAL
Lactational mastitis and breast abscess – diagnosis and management in general practice CLINICAL